Introduction
Compared with 2019, FAIR Health has observed significant increases in telemedicine services listed on insurance claims since the beginning of the COVID-19 pandemic.1 Similarly, virtual care provider Teladoc Health has reported a more-than 200% increase in total patient visits between Second Quarter 2019 and Second Quarter 2020.2 Telemedicine services have quickly changed from a lesser-used alternative delivery of treatment to a key medical tool. With possible benefits ranging from increasing efficiency of care to making specialists more easily accessible, this emerging option has the potential to positively affect an injured worker’s outcome.3 Telemedicine also faces limitations, such as the lack of face-to-face assessment, expensive implementation, and potential privacy concerns.
Prior to 2020, telemedicine services had slow adoption rates and low utilization in medical care. While NCCI data4 reflects the slow adoption of telemedicine in workers compensation (WC) insurance through 2019 (Chart 1), there are indications of a growing use of telemedicine in WC in 2020. However, will the increase in demand for telemedicine services be sustained long-term?
This article examines the state of telemedicine services prior to the COVID-19 pandemic by providing baseline information, a discussion of emergency changes, and insights on what the future may hold.
State of Telemedicine Prior to COVID-19
Many have touted the benefits of telemedicine services, from improving efficiencies to increasing medical accessibility in rural areas. However, medical practitioners have generally been slow to adopt telemedicine services. One possible reason may be applicable statutory and regulatory requirements governing the medical field’s use of telemedicine, including:
- Additional licensure requirements
- Permitted originating sites
- Regulations barring treatment for new patients
- Technology platform and HIPAA requirements
- Lower reimbursements
Telemedicine rules vary widely by state and may differ for injured workers receiving medical care under WC. Some states publish their own rules regarding telemedicine, while others rely on Medicare’s rules. In 2019, the Centers for Medicare & Medicaid Services (CMS) expanded the types of services that could be provided using telemedicine under Medicare, allowing more flexibility for administration and reimbursement. Despite this, the use of telemedicine under Medicare is still relatively limited. While CMS lists more than 8,000 procedures, less than 100 of these are approved to be delivered as a telemedicine service.
The allowable services most applicable to WC include evaluation and management (e.g., office visits) and psychiatry. On a countrywide basis, evaluation and management services account for the largest portion (69%) of telemedicine services provided by physicians. This percentage has remained relatively consistent over the most recent several years. Chart 2 shows the most common telemedicine services provided by physicians in 2019 and the corresponding share of telemedicine transactions.
Adapting Telemedicine Rules in Response to COVID-19
Increased reliance on telemedicine services has likely been largely driven by the desire to limit possible exposure to COVID-19, while maintaining continuity of care. States immediately started to act through issuance of guidance, emergency orders and reforms, encouraging the use of telemedicine for patients. Many orders were written with a focus on health insurers and did not explicitly include or exclude WC. Other announcements were not formally mandated, but instead were communicated via memos and bulletins that encouraged carriers to ensure that their telemedicine programs were adequate and robust enough to meet any increase in demand for processing telemedicine claims. While some orders introduced notable changes, others were temporary suspensions of preexisting rules that expired, in some instances, as soon as 120 days after the order was put into effect. Chart 3 highlights some of the most common provisions of these orders.
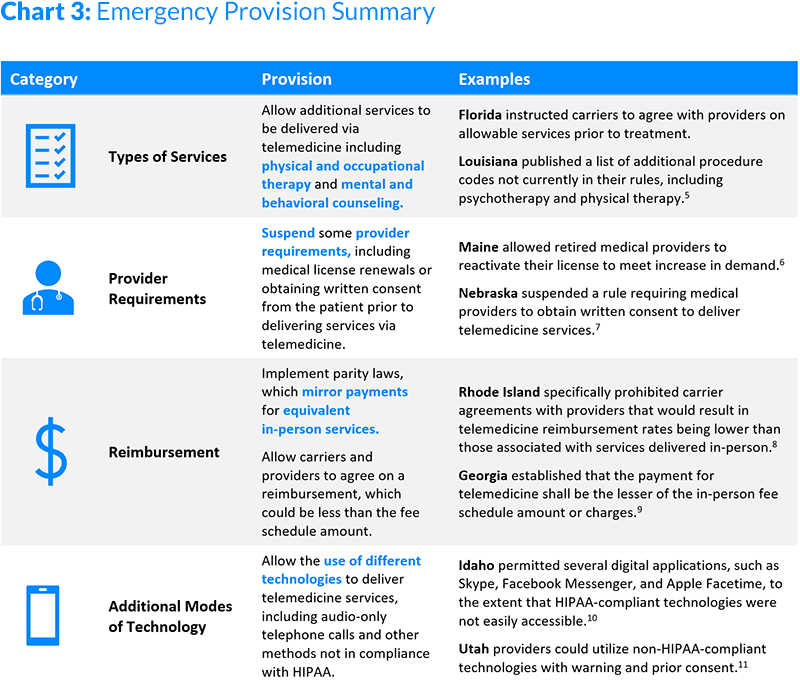
Other provisions seen across states include allowing out-of-state providers to deliver services within their scope of practice via telemedicine, suspending the requirement that telemedicine services could only be delivered to established patients, and allowing the homes of patients and medical providers to serve as originating and distant sites, respectively. In addition to individual state orders, the Coronavirus Aid, Relief, and Economic Security Act (CARES Act) set aside additional funds for healthcare providers to implement telemedicine systems, expanded Medicare’s telemedicine services, and increased Medicare’s flexibility for providing such services.12 Collectively, these changes have facilitated providers’ being able to deliver and patients’ receiving services via telemedicine with fewer barriers than experienced previously.
Conclusion
For the duration of the pandemic, it is expected that many individuals will utilize telemedicine and receive evaluation and management, physical therapy, and remote monitoring services in lieu of deferring medical services or receiving in-person treatment. It is also reasonable to believe that there may be a notable increase in remote physical therapy and mental health visits—where, previously, telemedicine was not commonly permitted. During the public health emergency, there was increased carrier outreach to inform providers and beneficiaries of available options. The effects of these educational measures could carry forward as providers become more familiar with delivering telemedicine services and the applicable governing requirements.
There continue to be many unanswered questions with respect to the state of telehealth services in WC:
- How will COVID-19 impact the utilization and accessibility of telemedicine services?
- Will utilization return to pre-pandemic levels or will telemedicine continue to be a common medical service delivery alternative?
- Will states choose to adopt permanent regulations regarding telemedicine in WC?
- How will telemedicine services be reimbursed?
NCCI will continue to monitor changes in telemedicine usage and how the utilization of telemedicine may impact the delivery of WC medical services.
This article is provided solely as a reference tool to be used for informational purposes only. The information in this article shall not be construed or interpreted as providing legal or any other advice. Use of this article for any purpose other than as set forth herein is strictly prohibited.
Glossary
Active Claim: A workers compensation claim for which there is at least one medical service provided during the referenced period.
Distant Site: The site where the physician or practitioner, who is providing the professional service, is located at the time the service, which is provided via a telecommunications system.
Fee Schedule: A list of codes and reimbursement amounts published by an individual jurisdiction or Medicare.
Originating Site: The location where a patient receives physician or practitioner medical services through a telecommunications system.
Service Year: A loss accounting definition in which experience is summarized by the calendar year in which the medical service was provided.
Telemedicine: The use of medical information exchanged via electronic communications to improve a patient’s clinical health status.