After years of rapid growth, claims costs are moderating ... but why?
Over the past two decades, the medical severity of workers compensation (WC) claims has cumulatively increased at a substantially faster pace than US healthcare costs. Medical services are a key factor in the WC system. They account for about 60% of all annual WC costs in the United States today—up from 40% in the early 1980s.
However, after a period of rapid increase, the growth in medical claims costs has recently moderated. Between Accident Years (AYs) 1995 and 2002, the annual growth stood at 9%. Between AYs 2009 and 2015, that growth rate was down to 1%.
AY 2015 was especially noteworthy. Claims costs actually decreased by 1%, the first year-over-year decline in more than 20 years. This was due, in part, to lower utilization of physician services. Costs grew again by 5% in 2016, but it wasn’t enough to negate the slower upward trend.
In this research brief, “Medical Costs Trends: Then and Now,” NCCI further explores this phenomenon. It compares medical cost drivers during rapidly increasing and relatively stable periods, and examines other possibly contributing factors.
Growing healthcare costs
WC medical severity rose rapidly from 1995 to 2002, outpacing the growth in US healthcare costs per capita during the same time frame. The growth slowed between 2002 and 2009 to a rate that was almost identical to the growth rate in US healthcare costs. That moderation continued between 2009 and 2015, when the growth in US healthcare costs actually exceeded the growth in claims costs.
The 2014–2015 decline in claims costs is due partly to lower costs for physician services, which include evaluations and management, medicine, surgery, and radiology. Physician services costs per claim fell 3% from 2014 to 2015, while hospital costs went up by 2%.
Contributing to that decrease was a 3% drop in physician utilization, which includes such factors as the number of physician office visits per claim, and the number and type of physician services provided during each visit. Average prices for physician services were unchanged from 2014 to 2015.
It is important to note that the type of injuries sustained in workers compensation were not a factor in the declining claims costs. Between 2012 and 2015, shares of different types of injuries—fractures, open wounds, sprains, and other conditions—held steady.
Increase of physician fee schedules and networks
Over time, another factor in moderating medical severity growth has been physician fee schedules, the most widely used mechanism for regulating WC medical payments. In 1979, only 12 states had a physician fee schedule. By 2016, that number had grown to 44 and, of those, 33 had implemented a Medicare-based physician fee schedule. Steady Medicare physician prices in recent years have helped control claims cost growth.
The growth of fee schedules is not exclusive to physicians. Many states have started using hospital fee schedules based on Medicare prices, and others are considering them.
Furthermore, most states have a prescription drug fee schedule, and many providers use pharmacy benefit management firms to help control WC drug costs.
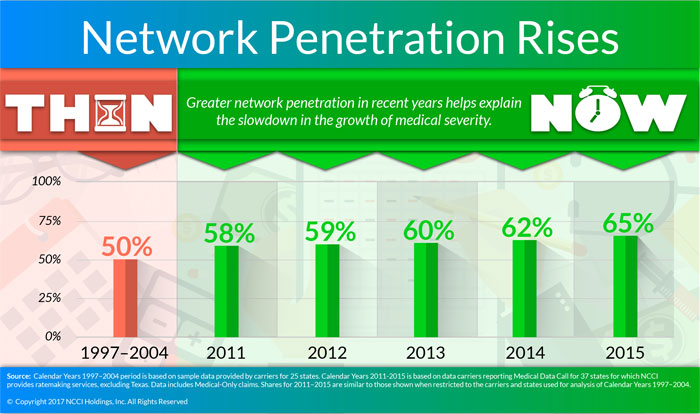
Also slowing claims cost growth is the increased presence of in-provider networks. The percentage of payments to in-network physicians has grown to 65% in 2015; between 1997 and 2004, it averaged about 50%. Physicians generally provide services in-network at a discount from similar services provided out-of-network. NCCI will look at this more closely in the future.
Medicare Set-Asides
Medicare Set-Asides (MSAs)—funds that are established to pay for future medical services due to work-related injuries that might otherwise be payable under Medicare—continue to put upward pressure on medical severity, and that pressure may have stabilized in the past few years. The Centers for Medicare & Medicaid Services (CMS) reviews proposed MSAs subject to certain eligibility criteria. They often require greater funding for the MSA than proposed. From 2010 to 2013, the gap between approved and submitted MSAs shrunk and, since then, remained relatively steady, as have the CMS-approved average amounts.
A look at the future
Finally, advances in medicine and medical technology are leading to treatments that could reduce or redefine permanent disability claims. People once bound to a wheelchair are, in some cases, now able to walk and improve their daily lives in ways not expected years ago. While some of the treatments could increase claims costs in the short term, some of the advances are cost-effective and could enable employees to return to work and regain control of their lives.
So why is it important to understand these medical cost trends?
Understanding the specific cost drivers in the WC system—and what leads to increases or decreases in costs—is essential for all system stakeholders. This data can help guide decisions that ensure that injured workers receive the high-quality care they need in the most effective and efficient manner possible, and ultimately foster a healthy WC system.
This article is provided solely as a reference tool to be used for informational purposes only. The information in this article shall not be construed or interpreted as providing legal or any other advice. Use of this article for any purpose other than as set forth herein is strictly prohibited.